Skin Cancer:
Early Detection
Saves Lives. Expert Care by Dr. Pang.
Expert skin cancer screening, diagnosis, and surgical treatment by Dr. Gateorn Pongarnar — Board-Certified Dermatologist & Dermatologic Surgeon at Dr. Pang Skin Clinic, Bangkok. In Thailand's tropical climate, professional skin checks are not optional — they are essential.

Board-Certified
Dermatologic Surgeon
Dermoscopy
Digital Imaging
Board-Certified Dermatologist
& Dermatologic Surgeon
Dermoscopy Screening
With Digital Imaging
Full Surgical Capabilities
Excision · Biopsy · Cryotherapy
5.0 Google Rating
Verified Patient Reviews
When Skin Cells Grow Out of Control
Skin cancer is the uncontrolled growth of abnormal skin cells, most often triggered by UV radiation from the sun. It is the most common cancer globally — and one of the most treatable when caught early. In Bangkok's tropical climate, with a UV Index of 10–14 (Extreme) year-round, regular professional skin checks are not optional. They are essential.
For Thai and Asian patients, BCC and SCC are the most common skin cancers due to chronic tropical UV exposure. While melanoma is less common in darker skin types, it does occur — and is particularly dangerous when it arises on palms, soles, or nail beds (acral lentiginous melanoma), where it is harder to detect.
"The difference between a routine check and a life-changing discovery is a single appointment. Early-stage skin cancer is highly curable. Late-stage skin cancer is not."
— Dr. Gateorn Pongarnar, M.D., Board-Certified Dermatologist & Dermatologic Surgeon
99%
Five-Year Survival Rate
Melanoma caught at its earliest stage
5–10%
Survival at Stage IV — why early detection matters
UV & Sun Exposure
The #1 driver of skin cancer. Bangkok's extreme UV (Index 10–14) creates chronic cumulative damage that builds over years.
Family History & Genetics
Personal or family history of skin cancer significantly increases risk of additional lesions. Annual screening is essential.
Immunosuppression & Age
Organ transplant recipients, those on immunosuppressive medications, and patients over 50 carry elevated risk for BCC and SCC.
Types of Skin Cancer
Each type of skin cancer has a distinct appearance, growth pattern, and treatment approach. Knowing what to look for — and acting quickly — is the single most important step you can take.
Basal Cell Carcinoma
Most CommonAppears as a flesh-colored, pearl-like bump or pinkish patch on sun-exposed skin. BCC grows slowly and rarely spreads — but left untreated, it invades surrounding tissue and can cause significant destruction to the face, nose, and ears.
Recommended Treatment
Surgical excision · Mohs surgery (facial areas) · Cryotherapy · Topical imiquimod / 5-FU
Squamous Cell Carcinoma
Second Most CommonRed, firm bumps or scaly patches that may heal and reopen. More aggressive than BCC and carries metastatic potential — it can spread to lymph nodes and organs. Excellent outcomes (95–98%) with early surgical removal.
Recommended Treatment
Surgical excision · Mohs surgery · Cryotherapy · Immunotherapy (advanced stage)
Melanoma
Most DangerousThe deadliest form of skin cancer — but also highly curable when detected early. Develops in existing moles or as a new dark spot. Any changing mole deserves immediate professional evaluation. Use the ABCDE rule to self-monitor.
Recommended Treatment
Excisional biopsy · Sentinel lymph node biopsy · Immunotherapy · BRAF-targeted therapy (advanced)
Actinic Keratosis
Pre-Malignant — Act NowRough, scaly patches on sun-exposed skin from cumulative UV damage. Not yet cancer — but without treatment, actinic keratosis can progress to invasive squamous cell carcinoma. Easily and effectively treated when caught early.
Recommended Treatment
Cryotherapy · Topical 5-FU or imiquimod · Photodynamic therapy (PDT)
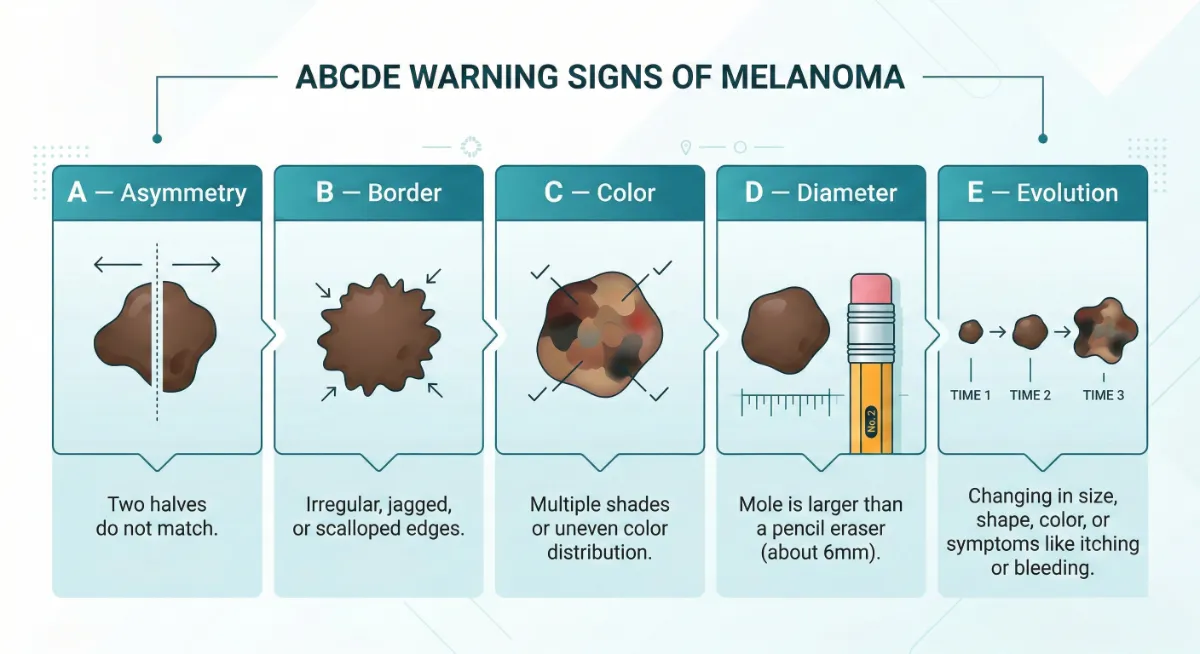
Could It Be Melanoma? Check ABCDE.
The ABCDE rule is the gold-standard method for identifying potentially malignant moles and lesions. Any single warning sign warrants professional evaluation — do not wait.
Asymmetry
One half of the lesion does not match the other in shape or size. Normal moles are symmetrical.
Border
Irregular, ragged, notched, or blurred edges. Benign moles have smooth, well-defined borders.
Color
Multiple shades — brown, black, red, grey, or dark blue within the same lesion. Uniform color is reassuring.
Diameter
Larger than 6 mm — roughly the size of a pencil eraser. Melanomas are often larger at diagnosis, but can be smaller.
Evolution
Any change in size, shape, or color — or a new symptom such as bleeding, itching, or crusting. Evolution is the most important warning sign.
If any lesion shows one or more of these signs — book an evaluation today.
Early-stage melanoma has a 99% five-year survival rate. Do not dismiss warning signs as cosmetic concerns.
Book a Lesion EvaluationSee Beyond the Surface with Dermoscopy
Dermoscopy is a non-invasive diagnostic tool using polarized magnification to reveal subsurface structures invisible to the naked eye — allowing Dr. Pang to assess pigmentation depth, vascular patterns, and lesion architecture before any biopsy is performed.
Distinguishes Benign vs. Malignant
Identifies lesion characteristics that guide clinical decision-making
Improved Diagnostic Accuracy
57.8% (naked eye) → 75.9% (trained dermoscopy)
Reduces Unnecessary Biopsies
Confident differentiation means fewer invasive procedures
Digital Imaging & Tracking
Lesion changes documented over time for ongoing monitoring
Biopsy Methods at Dr. Pang Skin Clinic
Shave Biopsy — Superficial raised lesions; no stitches required
Punch Biopsy — Full-thickness core; 1–2 stitches; deeper lesions
Excisional Biopsy — Complete lesion removal; gold standard for melanoma

Screening takes just 20–30 minutes.
Non-invasive · No pain · No preparation required
Precise Treatment. Maximum Cure Rate.
Dr. Pang selects the most appropriate treatment based on cancer type, size, location, depth, and your individual health profile. Every plan is tailored — not template-driven.
Surgical Excision
Primary TreatmentComplete removal of skin cancer with a clear margin of healthy surrounding tissue. Tissue is submitted to a dermatopathologist for histological confirmation of clear margins.
Cryotherapy
Office-BasedLiquid nitrogen freezes and destroys precancerous lesions and superficial skin cancers. A fast, effective in-office procedure with minimal recovery. May require repeat sessions for complete clearance.
Skin Biopsy
Diagnostic Gold StandardPunch, shave, or excisional biopsy performed under local anesthesia. Tissue sample sent to dermatopathologist for definitive diagnosis. Results typically available within 1–2 weeks.
Topical Therapy
No SurgeryImiquimod (Aldara) or 5-fluorouracil (5-FU) cream for superficial BCC and actinic keratosis where surgery is not preferred or in patients with multiple lesions. Applied at home under medical supervision.
Mohs Surgery
Referral AvailableLayer-by-layer removal with real-time microscopic margin assessment. 99% cure rate for new BCC/SCC. Optimal for cosmetically sensitive areas (face, nose, ears, eyelids). Dr. Pang coordinates referral when indicated.
Co-Management & Referral
For advanced or complex cases requiring immunotherapy, radiation, or multidisciplinary oncology care, Dr. Pang provides co-management and coordinates referrals to the appropriate specialists.
Advanced BCC (Vismodegib) · Advanced SCC (Cemiplimab) · Advanced Melanoma (Anti-PD-1 / BRAF therapy)
What to Expect at Dr. Pang Skin Clinic
From your first screening to confirmed clear margins — here is exactly what your skin cancer care journey looks like with Dr. Pang.
Skin Cancer Screening
Full-body visual examination combined with dermoscopy of any suspicious lesions. Digital imaging of concerning areas.
20–30 minutes
Lesion Evaluation
ABCDE analysis, dermoscopy pattern interpretation, and clinical assessment. Dr. Pang explains findings and discusses next steps.
Same visit
Biopsy (If Indicated)
Punch, shave, or excisional biopsy under local anesthesia. Painless procedure. Sample sent to dermatopathologist for definitive diagnosis.
Results in 1–2 weeks
Results & Treatment Plan
Dr. Pang reviews pathology, explains findings clearly, and recommends the most appropriate treatment approach for your specific case.
Personalized plan
Treatment & Follow-Up
Surgical excision, cryotherapy, or topical protocol with confirmed clear margins and regular monitoring to detect any recurrence early.
Ongoing monitoring
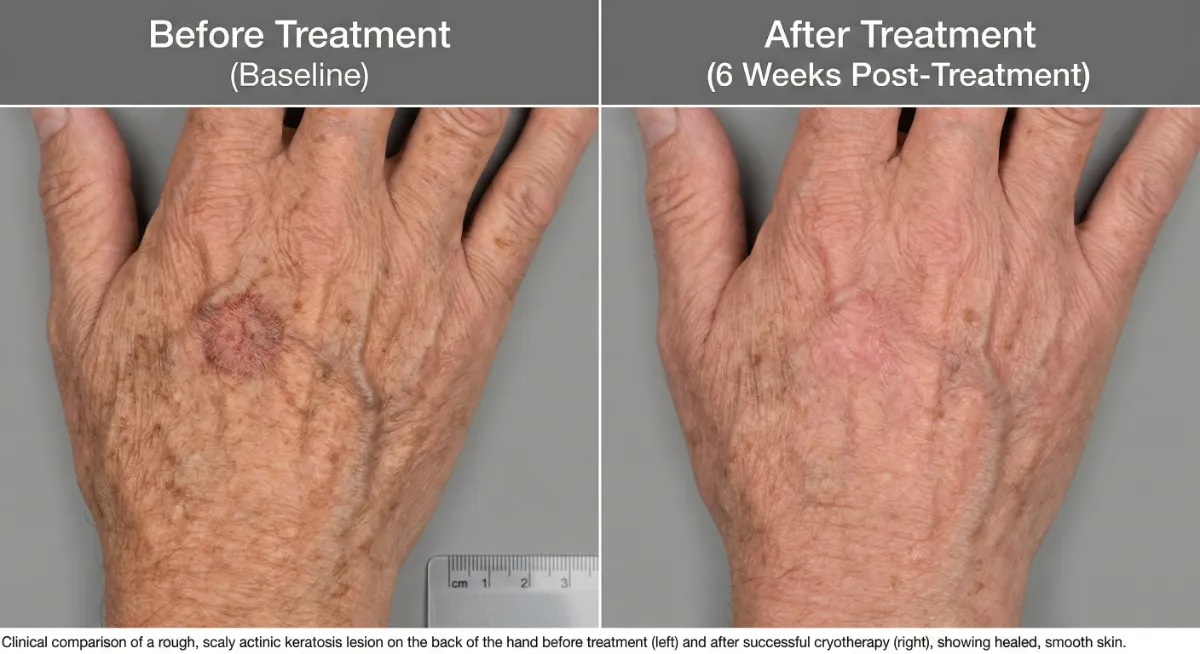
Treatment Results. Real Patients.
Effective skin cancer treatment leaves minimal trace when performed by an experienced dermatologic surgeon. Results below represent actual patients treated at Dr. Pang Skin Clinic. Individual results may vary.
Dr. Pang — Your Skin Cancer Specialist
Dr. Gateorn Pongarnar, M.D. is a board-certified dermatologist and dermatologic surgeon with over 13 years of clinical experience. She provides comprehensive skin cancer care: from non-invasive dermoscopy screening through to surgical excision, biopsy, cryotherapy, and co-management of complex cases.
Dr. Pang believes that in Bangkok's extreme UV environment, proactive skin cancer screening is one of the highest-value health investments you can make. Her approach: thorough, honest, and patient-first.

13+
Years of Clinical Experience
5★
Google Reviews Average
2025
EndoliftX Clinic of the Year Asia-Pacific
FDA
Approved Treatment Protocols
Protect Your Skin. Reduce Your Risk.
Bangkok's tropical UV environment means year-round protection is non-negotiable. These evidence-based practices significantly reduce your lifetime skin cancer risk.

Daily SPF 50+ Sunscreen
Broad-spectrum SPF 50+ applied every morning. Reapply every 2 hours when outdoors. Tinted sunscreens with iron oxide offer additional protection against visible light.
Avoid Peak Sun Hours
UV intensity peaks between 10 AM and 4 PM. Seek shade, schedule outdoor activities for early morning or late afternoon, and limit cumulative exposure.
UV-Protective Clothing
UPF 50+ clothing, wide-brimmed hat, and UV-blocking sunglasses. Physical barriers are more reliable than sunscreen alone for prolonged outdoor exposure.
Monthly ABCDE Self-Exams
Examine your entire skin once a month — including scalp, between toes, and nail beds. Use a mirror or ask a partner for areas you cannot see. Know your moles.
Annual Professional Screening
Annual full-body dermoscopy screening by a board-certified dermatologist. More frequent (every 6 months) if you have fair skin, family history, or numerous moles.
Your Prevention Starts Here
A professional skin check is the most important step you can take today. Dr. Pang provides thorough assessments with clear, honest communication.
Book Your ScreeningYour Questions, Answered
Once per year for all adults — this is the baseline recommendation. More frequent checks (every 6 months) are advised if you have: fair skin or Fitzpatrick type I–II, personal or family history of skin cancer, many moles (more than 50), a history of heavy sun exposure, or immunosuppression. Dr. Pang will recommend a monitoring schedule appropriate for your individual risk profile.
BCC and SCC are common in Thailand due to chronic, extreme tropical UV exposure (UV Index 10–14 year-round). Melanoma is less common in Asian skin types — Asian skin has higher baseline melanin providing some UV protection — but it does occur. When melanoma develops in Asian patients, it more commonly appears on palms, soles, or nail beds (acral lentiginous melanoma), where it is harder to detect and often diagnosed at a later stage. This makes professional screening especially important.
A full-body visual examination by Dr. Pang — examining the skin from scalp to toes, including commonly missed areas (between toes, nail beds, scalp). Suspicious lesions are evaluated with dermoscopy, a polarized-light magnification tool that reveals lesion architecture invisible to the naked eye. Digital images are taken of any lesions that warrant monitoring. The entire process is non-invasive, painless, and typically takes 20–30 minutes.
Surgical excision and biopsy are performed under local anesthesia. You will feel pressure during the procedure but not pain. After the anesthesia wears off, mild discomfort and some swelling are normal for 24–48 hours, well-managed with standard analgesics. Stitches are typically removed after 5–14 days depending on location. Most patients return to normal activities the following day.
Long-standing moles that are stable are generally reassuring — but not absolutely safe. The most critical warning sign is evolution (the "E" in ABCDE): any change in size, shape, color, or new symptoms such as bleeding, itching, or crusting in any lesion, old or new, warrants professional evaluation. Additionally, some melanomas can arise in normal-appearing skin without a pre-existing mole. Annual professional screening remains the safest approach regardless of lesion age.
Benign moles (nevi) are stable, symmetrical, evenly colored, and have clear borders — they appear in childhood or early adulthood and do not change. Skin cancer, by contrast, shows asymmetry, irregular borders, multiple colors, large diameter, or evolving characteristics. The only way to definitively distinguish a suspicious mole from early melanoma is dermoscopy and, when necessary, biopsy with histological analysis. Self-assessment using the ABCDE rule is a useful first step, but professional evaluation by a board-certified dermatologist is the gold standard.
After surgical excision, the specimen is sent for histological confirmation of clear margins. Follow-up appointments are scheduled to check healing and wound management. Depending on the cancer type and stage, regular skin checks every 3–6 months are recommended for at least the first 2–3 years, as a history of skin cancer significantly increases the risk of developing additional lesions. Sun protection becomes critical and non-negotiable post-treatment.
Don't Wait for a Warning Sign.
Schedule Your Screening Today.
Skin cancer caught early is highly treatable. A 20-minute dermoscopy screening with Dr. Pang is one of the most valuable investments in your health — especially in Bangkok's extreme UV environment.